Diabetic Foot Complications at Foot and Ankle Rehabilitation
Diabetes can quietly damage nerves and circulation, raising the risk of wounds, infection, and ulceration. Early podiatry input dramatically reduces complications.
At Foot and Ankle Rehabilitation, we provide comprehensive diabetic foot screening, preventive care, wound management, footwear advice, and orthotics—working closely with your GP and diabetes team.
What are Diabetic Foot Complications?
Diabetes can lead to significant changes in the feet due to its effects on nerves, circulation, and wound healing. Over time, elevated blood glucose levels may damage the peripheral nerves (peripheral neuropathy) and blood vessels (peripheral arterial disease), leaving the feet vulnerable to injury, ulceration, and infection.
Without early intervention, these complications can progress to serious infection, gangrene, or amputation. Regular podiatry care is a cornerstone of diabetic management, helping to prevent complications before they develop.
At Foot and Ankle Rehabilitation, we provide specialist diabetic foot assessments, preventive care, and treatment, with access to PHO-funded appointments where eligible.
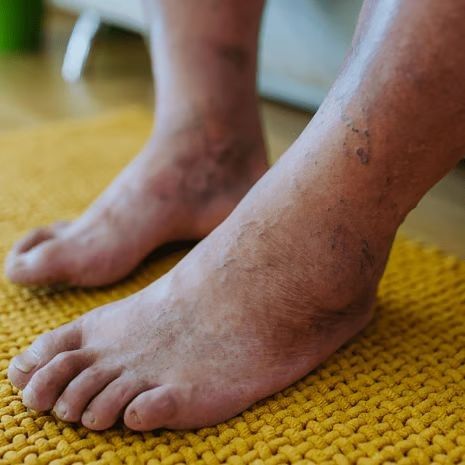
Causes & Risk Factors
Peripheral neuropathy – nerve damage leading to numbness, burning, tingling, or loss of protective sensation
Peripheral arterial disease (PAD) – reduced circulation impairing healing and increasing ulcer risk
Foot deformities – bunions, hammer toes, flat feet causing abnormal pressure points
Callus and skin breakdown – predisposing to ulceration
Poor footwear – rubbing or pressure leading to unnoticed wounds in neuropathic patients
High blood glucose levels – impairing wound healing and immune function
History of ulcers or amputation – strongest risk factor for recurrence
Smoking, kidney disease, hypertension – further increasing risk
Treatment at Foot and Rehabilitation
Preventive care – regular podiatry appointments for nail care, callus removal, and footwear review
Custom orthotics and insoles – offloading pressure points to prevent ulcers
Footwear prescription – diabetic-friendly shoes with depth, cushioning, and minimal seams
Wound care – dressing and offloading strategies for active ulcers
Shockwave therapy (ESWT) – for associated tendon or musculoskeletal pain in diabetic patients (safe when indicated)
Education – self-care techniques, daily foot checks, and early warning signs
Multidisciplinary collaboration – communication with GPs, endocrinologists, diabetes nurses, and vascular specialists
PHO-funded care – through contracts with Pinnacle, East Health Trust, and ProCare, patients may be eligible for subsidised or funded appointments following GP referral
Symptoms
Numbness, tingling, or burning sensations in the feet
Loss of protective sensation – inability to feel pressure, heat, or injury
Poor wound healing or recurrent infections
Skin changes – dryness, cracks, or colour changes
Foot deformity or pressure-related callus build-up
Ulcers on weight-bearing areas (toes, ball of foot, heel)
Pain at rest or during walking, which may indicate poor circulation
Diagnosis
At Foot and Ankle Rehabilitation, our diabetic foot assessment includes:
Vascular testing – palpation of pulses, Doppler ultrasound if indicated
Neurological testing – 10g monofilament, tuning fork vibration testing, light touch, temperature sensation
Footwear review – to identify risk of rubbing or pressure areas
Skin and nail evaluation – identifying callus, fungal infection, cracks, or wounds
Biomechanical assessment – to detect deformities increasing ulcer risk
Risk classification – determining whether the patient is low, moderate, or high risk and setting review frequency accordingly
Contact us to learn more about Diabetic Foot Complications treatment
If you are dealing with Diabetic Foot Complications, our team can help you find the most suitable Foot and Ankle Rehabilitation clinic for assessment, diagnosis, and treatment support.
Whether your symptoms are affecting walking, running, exercise, or daily comfort, we can guide you towards the right clinician and the right next step for your care.
Treatment options are available across Pinehill, Smales Farm, Remuera, Botany, Hamilton East, Hamilton Central and Bethlehem

Podiatrist pricing and availability
Pricing for Diabetic Foot Complications assessment and treatment can vary depending on your consultation, the severity of your symptoms, the treatment approach recommended, and whether ongoing podiatry or rehabilitation care is required.
Your Foot and Ankle Rehabilitation clinician will assess your tendon, identify the contributing factors to your pain, and explain the most appropriate treatment plan based on your symptoms, activity level, and recovery goals.
To learn more about our podiatrists and current pricing, use the links below:
10,000+
Appointments delivered across our clinics, helping patients improve foot health, mobility, and long-term outcomes.
7 Clinics
Conveniently located across Auckland, Hamilton, and Tauranga, making it easy to access a podiatrist near you.
30+ Treatments
Comprehensive podiatry services including fungal nail care, ingrown toenail treatment, rehabilitation, and general foot care.
Diabetic Foot Complications – FAQs
Why are feet at risk in diabetes?
Diabetes can damage nerves (neuropathy) and blood vessels (circulatory disease). This means patients may not feel injuries and have reduced ability to heal, creating a higher risk of ulcers and infection.
What is peripheral neuropathy?
Peripheral neuropathy is nerve damage caused by long-term high blood glucose levels. It can cause numbness, tingling, burning pain, or loss of protective sensation in the feet, making injuries go unnoticed.
What is peripheral arterial disease (PAD)?
PAD occurs when the arteries supplying the legs and feet become narrowed or blocked. This reduces blood flow, leading to pain, delayed healing, and higher risk of ulcers and infection.
How often should I have my feet checked if I have diabetes?
At minimum, diabetic patients should have an annual foot screening. High-risk patients (with neuropathy, PAD, ulcers, or deformity) require more frequent checks, often every 3–6 months.
What shoes are best for diabetic feet?
Extra depth and width
Soft, cushioned lining with no seams
Firm midsole for stability
Custom insoles or orthotics to reduce pressure points
Can diabetes cause foot ulcers?
Yes. Ulcers are common in diabetes, particularly in patients with neuropathy or poor circulation. Ulcers must be treated urgently to prevent infection and serious complications.
Are diabetic foot complications preventable?
Yes. With good blood sugar control, regular podiatry visits, correct footwear, and self-care, most serious diabetic foot problems can be prevented.
What funding is available for diabetic foot care?
Foot and Ankle Rehabilitation holds PHO contracts with Pinnacle, East Health Trust, and ProCare. Patients referred by their GP may be eligible for funded or subsidised appointments for diabetic foot assessments and care.
When should I see a podiatrist urgently?
If you notice an ulcer, open wound, swelling, redness, pus, or sudden change in sensation, you should seek urgent podiatry or GP assessment. Early treatment can prevent amputation.

Why Choose Foot and Ankle Rehabilitation?
Foot and Ankle Rehabilitation provides specialist diabetic foot care, combining podiatry and physiotherapy expertise with access to funded care pathways. We focus on prevention, education, and advanced treatment, helping patients with diabetes protect their feet and maintain independence.
With clinics in Rosedale, Takapuna, Remuera, Botany, Hamilton, and Tauranga, expert diabetic foot care is available across New Zealand.

